[lwptoc]
Many people are confused about dementia and Alzheimer’s disease.
What are the four major types of dementia? Other rare forms of dementia?
You can find all the answers in this post.
Also included are their diagnoses, treatments, and tips on caring for your loved ones.
Chapter 1. Dementia and Alzheimer’s Disease
Among various types of dementia, Alzheimer’s is the most common one.
As the population ages, 150 million more people will suffer from dementia in 30 years worldwide.
Are you at risk?
Let’s find out.
Dementia is a type of brain disease that causes long-term and progressive deterioration in thinking and memory. There are four significant types of dementia, and Alzheimer’s disease accounts for most of the cases.

Dr. Alois Alzheimer
Alzheimer’s disease got its name from Dr. Alois Alzheimer, a German psychiatrist who discovered the first recorded case of this disease.
Dementia affects people of all ages, but is most common in older adults.
More than 50 million people of all ages are living with dementia globally. According to the WHO, the cases of dementia may triple by 2050.
Unfortunately, no one test can confirm a diagnosis of dementia. To do this, doctors must rely on a comprehensive assessment, which includes cognitive tests, a physical examination, brain imaging, and blood tests.

Image by Yerson Retamal from Pixabay
The dementia ICD-10 (The International Classification of Diseases version 10) code is F03.90.
Understanding Different Types of Dementia
There are many types of dementia, each with its own symptoms.
The most common types are Alzheimer’s disease, vascular dementia, Lewy body dementia, and frontotemporal dementia.
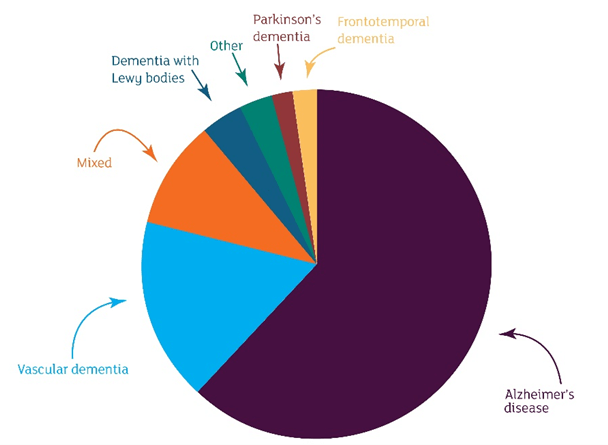
Credit Alzheimer’s Research UK
Alzheimer’s begins as a loss of memory. It accounts for 60-80% of all cases.
The brain degeneration is Alzheimer’s main feature, affecting people’s functioning.
Vascular dementia is responsible for up to 20% of dementia cases. It is caused by damage to the blood vessels that supply the brain.
Lewy body dementia causes 10 to 15% of dementia. The accumulation of Lewy bodies in the brain leads to symptoms, including memory loss, hallucinations, and movement disorders.
Frontotemporal dementia accounts for only contributes to 2% of dementia cases—the frontal and temporal lobes of the brain degenerate, causing various symptoms.
How Many People Worldwide Have Dementia and the Cost
There are approximately 47.5 million people worldwide who have dementia. The cost of treatment varies by country, but the average annual cost of care is roughly $8,000.
In the US, there are about 5.8 million people with dementia. That number may double, and the cost of caring for those with dementia is projected to reach $1.1 trillion by 2050.
What Are My Chances of Getting Alzheimer’s and Dementia?
Suppose you have a first-degree relative, like a parent, brother, or sister, with Alzheimer’s disease. In that case, you may have a two to three-fold increased risk of developing the disorder compared with others.
However, old age is the most significant risk factor for all forms of dementia.
Chapter 2. Alzheimer’s Disease
Does the APOE4 gene cause Alzheimer’s? Is memory loss equal to senile dementia?
This section of the article will explain all these points.
In addition to the diagnosis and treatment of dementia, caregivers can also benefit from caregiving tips.
Image by S. Hermann / F. Richter from Pixabay
What Are the Causes of Alzheimer’s?
The causes of Alzheimer’s disease are not fully understood.
However, certain risk factors have been identified, including genetic predisposition, lifestyle choices, and underlying health conditions.
Among them, around one in every six cases of Alzheimer’s disease can be related to genetics.

Image by Ursula Di Chito from Pixabay
Yes…
It could be the genes…
One of the most significant genetic risk factors for Alzheimer’s disease is the apolipoprotein E4 (APOE4) gene.
If you have one copy of this gene, you have a two to three-fold higher chance of developing Alzheimer’s. If you have two copies, the risk is eight to twelve-fold higher.
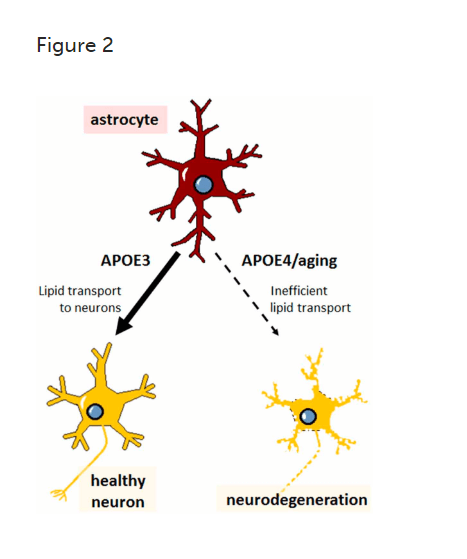
Credit Celia G. Fernandez, frontiers
More (APOE4) is less (brain)…
But having two copies of APOE4 does not mean you are guaranteed to have Alzheimer’s disease. Nonetheless, family history plays a significant role in Alzheimer’s disease development.
Lifestyle choices such as smoking, drinking too much alcohol, and not exercising can also increase the risk of developing Alzheimer’s disease.
Chronic diseases like diabetes, high blood pressure, and high cholesterol are risk factors too.

Image by Michal Jarmoluk from Pixabay
Lifestyle matters a lot…
Inside the Alzheimer’s brain, the tau protein tangles INSIDE neurons, and amyloid plaques formed BETWEEN neurons are the two main pathological features. Chronic inflammation and blood vessel problems also contribute to the damage to the dementia brain.
What Are the Symptoms of Alzheimer’s
The symptoms of Alzheimer’s disease can vary from person to person.
Some common symptoms include:
- Memory loss.
- Difficulty performing familiar tasks.
- Problems with language and communication.
- Disorientation and confusion about time and place.
- Changes in mood and personality.
- Decreased motivation.
Additionally, as the disease progresses, individuals may experience more severe symptoms, such as hallucinations and delusions.
What Are the Stages of Alzheimer’s
There are four general stages of Alzheimer’s disease: Pre-clinical, mild (early-stage), moderate (middle-stage), and severe (late-stage).

Credit McMaster University
Pre-clinical is the earliest stage where brain changes occur, but there are no noticeable symptoms.
Mild (early-stage) is when someone begins to experience memory lapses and other problems with thinking and cognition.
(Senile degeneration of the brain and senile dementia were terms once used on people with mild Alzheimer’s disease.)
Moderate (middle-stage) is characterized by memory loss and cognitive issues that interfere with daily life, such as difficulty carrying on a conversation or recognizing familiar faces.
Severe (late-stage) is the most advanced stage of Alzheimer’s disease, where individuals lose the ability to communicate and entirely depend on others for their care.
How to Diagnose Alzheimer’s
No test can confirm the diagnosis of Alzheimer’s disease.
A diagnosis typically involves a combination of medical and cognitive assessments, as well as input from family members or caregivers.
Some medical and cognitive assessments can rule out other potential causes of dementia symptoms, such as thyroid problems, vitamin deficiencies, or depression.
One common assessment tool is the Mini-Mental State Examination (MMSE), which evaluates cognitive function in areas such as memory, language, attention, and visuospatial skills. A score of 24 or below on the MMSE indicates the presence of dementia.
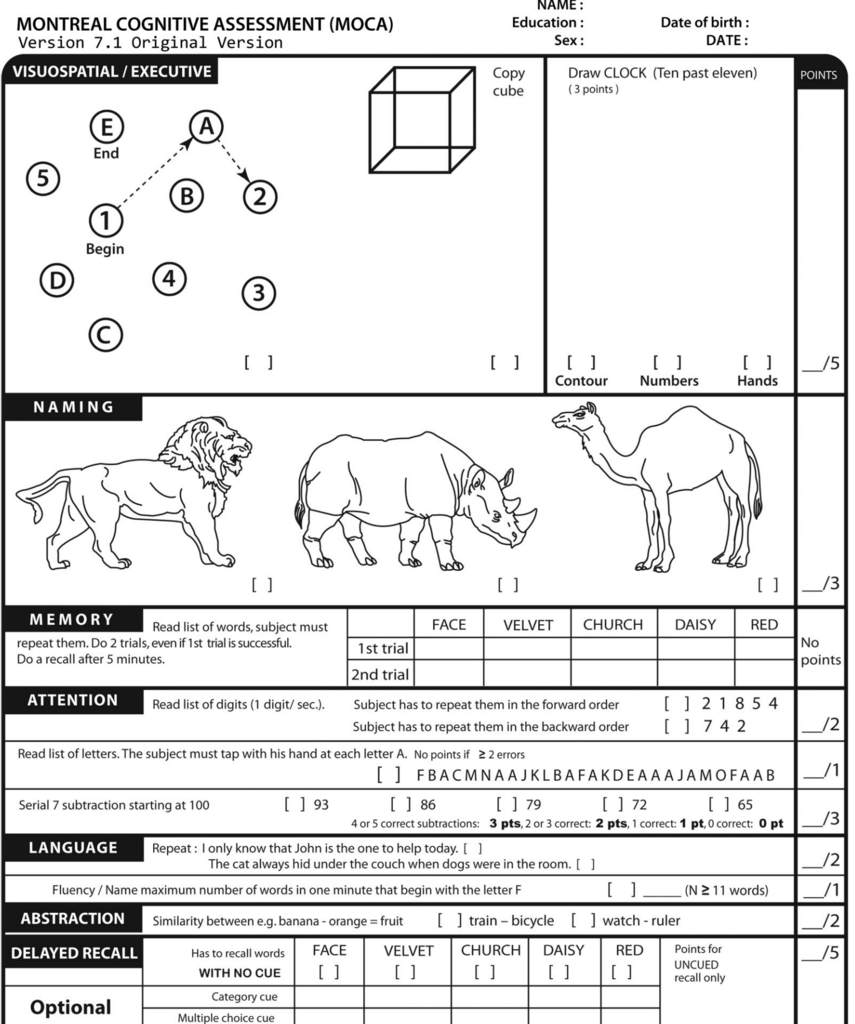

Other helpful tests include:
- Brain imaging scans (such as MRI or PET scans with a radioactive diagnostic agent, Amyvid).
- Genetic testing.
- Neuropsychological testing.
Alzheimer’s Disease Treatment
There is no cure for Alzheimer’s disease.
But some treatments can slow its progression and improve the quality of life. They aim to manage behavioral symptoms, relieve anxiety, and help patients maintain independence.
Medications can temporarily improve mental function and reduce behavior problems such as aggression or agitation.
Types of medications for Alzheimer’s treatment are:
Cholinesterase inhibitors: Donepezil (Aricept), rivastigmine (Exelon), and galantamine (Reminyl).
These drugs increase levels of acetylcholine, a neurotransmitter essential for memory and cognitive function.
Side effects include nausea, vomiting, diarrhea, and loss of appetite.
Antipsychotic medications: Quetiapine (Seroquel), risperidone (Risperdal), or olanzapine.
They treat behavioral problems associated with Alzheimer’s disease and Lewy body dementia.
However, antipsychotics may cause strokes in the elderly. Doctors will only prescribe this treatment if all other options have failed.
Memantine: This medication reduces damage caused by the overactivity of glutamate in Alzheimer’s disease.
Memantine can help improve thinking skills slightly, but there are no significant improvements in memory or behavior. It should be used with others as a treatment strategy.
Common side effects include confusion, dizziness, and sleepiness. There are rare cases of hallucinations, primarily if used with cholinesterase inhibitors together.
*Talk to your doctor for medical advice.
Tips for Family and Caregivers
If you provide care for individuals with Alzheimer’s, you may need extra patience and understanding.
The person may have difficulty communicating their feeling. A calm approach, a safe environment, and the willingness to help are essential for a caring relationship.

Credit caropat from pixabay
I need your help
Sooner or later, you may encounter common behavior issues in Alzheimer’s, like wandering, aggression, and delusions.
Wandering is when a person with Alzheimer’s gets up and walks around without any particular destination.
This can be a safety concern, as the person may not be aware of their surroundings and could get lost.
If you are caring for someone prone to wandering, try these measures to create a safe environment:
- Remove hazards from home.
- Make sure they are always supervised.
- Get a GPS tracking device.
- ID bracelets can help authorities locate the person if they get lost.
Aggression is when a person with Alzheimer’s disease becomes angry or violent. It may be a response to feeling frustrated or confused.
If you are caring for someone with aggressive behavior, these tips may help:
- Stay calm and de-escalate the situation.
- Distract them with another activity.
- Leave the person alone if your presence exacerbates the aggression.
- Consult with the person’s doctor about potential treatments.
A delusion is an untrue belief that a person holds despite evidence to the contrary.
People with Alzheimer’s disease may develop delusions as the disease progresses. For example, they may believe that their spouse is cheating on them or that someone is stealing their stuff.
If you are caring for someone with delusions, try these tips:
- Don’t argue or try to convince.
- Give a simple answer or redirect their focus.
- Consult with the person’s doctor about potential treatments.
If you are overwhelmed or need more advice, support groups are available for caregivers of people with Alzheimer’s.
Chapter 3. Frontotemporal Dementia (FTD)
The most distinctive characteristic of frontotemporal dementia is odd behavior.
Most cases start at age 45-65, relatively younger than Alzheimer’s.
It worsens steadily and brings unique challenges for caregivers dealing with behavior and movement issues.
What Are the Causes of Frontotemporal Dementia?
In most cases, the causes of frontotemporal dementia are unknown.
Genetic factors may play a role because people with a family member who has FTD are more likely to develop such a disorder.
Researchers have also found that some gene mutations can lead to FTD, like Pick’s dementia.
Traumatic brain injury is another factor that can increase the risk.

What Are the Symptoms of Frontotemporal Dementia?
The symptoms of frontotemporal dementia can vary depending on which brain area is affected.
However, common symptoms may include changes in personality and behavior, language and speech problems, and difficulties with motor skills.
Personality and behavior changes include:
- Apathy
- Irritability
- Impulsivity
- Disinhibition
- Agitation
Language and speech problems include:
- Trouble finding the right words to say (verbal apraxia)
- Saying meaningless words (agrammatism)
- Slow or halting speech (dysarthria)
- Difficulty understanding what others are saying (receptive aphasia)
Difficulty with motor skills is:
- Clumsiness
- Tremors
- Difficulty walking or moving
What Are the Stages of Frontotemporal Dementia?
The stages of frontotemporal dementia are:
1. Early stage
In the early stage, people with frontotemporal dementia may have difficulty maintaining social boundaries and norms.
They may act out of character, being impulsive and careless. Families and loved ones may also perceive the person as uncaring and selfish, leading to a loss of interest in everything. This is the behavioral variant of frontotemporal dementia (bvFTD).
Some individuals may struggle to understand words or speak coherently. This type is called primary progressive aphasia; some mistakenly call it “aphasia dementia.”
2. Middle stage
As the condition progresses, behavioral and language symptoms continue to worsen and occur more frequently.
Additionally, they may require more assistance with their activities of daily living (ADLs), including bathing, dressing, and grooming.
3. Late stage
In this stage, people with FTD often lose the ability to communicate, and their memory is affected.
They may be completely immobile and require full-time care. Eventually, they may die of infections such as pneumonia.
How to Diagnose Frontotemporal Dementia?
There is no definitive test for diagnosing frontotemporal dementia.
Doctors typically begin with a comprehensive medical history, a physical examination, and a neurological examination.
They may order tests to rule out other possible causes, such as a stroke or tumor.
Imaging tests, such as MRI or CT scans, are practical for assessing changes in the brain. A PET scan can sometimes be helpful in diagnosis as well.
In rare cases, a biopsy of brain tissue may be done to confirm the diagnosis.
Frontotemporal Dementia Treatment
There is currently no cure for frontotemporal dementia. The overall goal is to manage the symptoms.
How to manage behavioral symptoms?
Creating a routine: Having a set daily routine can help to minimize confusion and anxiety.
Simplifying choices: Offering the person a limited number of choices can help to reduce frustration and confusion—for example, two breakfast options instead of six.
Promoting social interaction: Engaging in social activities, such as talking with friends or going for walks, can reduce feelings of isolation and loneliness.
Managing stress: Stress can worsen the symptoms of frontotemporal dementia. Therefore, it is crucial to reduce stress in patients’ lives (e.g., through relaxation techniques or exercise).
How to manage language symptoms?
Speech therapy: A speech therapist can help patients improve their communication skills. This may involve working on pronunciation, grammar, and vocabulary.
Augmentative and alternative communication (AAC): AAC refers to any type of nonverbal communication, such as hand gestures or sign language. AAC can be used to supplement or replace speech in patients with frontotemporal dementia.
How to manage movement symptoms?
Physical therapy: A physical therapist can help patients improve their strength and flexibility. This may involve exercises, stretching, and massage.
Assistive devices, such as walkers or grab bars, can help patients with frontotemporal dementia stay mobile and independent.
Medications: Parkinson’s disease medications and antidepressants may sometimes help relieve movement symptoms.
Tips for Family and Caregivers
If you are a caregiver for someone with frontotemporal dementia, make sure to take care of yourself physically and emotionally.
- Get yourself a health checkup regularly.
- Ask for help from family and friends with life tasks like grocery shopping.
- Enjoy leisure time away from caregiving.
- Utilize short-term care services, such as respite and adult day care centers.
- Join support groups for FTDs.
- Find resources from non-profit organizations and research centers.
- Arrange for long-term care facilities when the care is too demanding, such as group homes, assisted living facilities, or nursing homes.
Chapter 4. Lewy Body Dementia
Lewy body dementia is related to Parkinson’s disease via the protein called Lewy bodies.
Of course, they both affect people’s movement.
It progresses much faster; patients typically survive five to seven years from diagnosis.
Our goal is to help individuals live a longer, more fulfilling everyday life…
What Are the Causes of Lewy Body Dementia?
Lewy bodies are protein deposits that build up in nerve cells and are a hallmark of Parkinson’s disease.
It is thought that these same protein deposits may also contribute to the development of Lewy body dementia.

Dementia with Lewy bodies. Wikipedia.
What Are the Symptoms of Lewy Body Dementia?
The symptoms of Lewy body dementia may include:
- Problems with thinking, reasoning, and judgment.
- Hallucinations.
- Changes in sleep patterns.
- Parkinson’s disease-like movement problems.
- Fluctuating levels of alertness and attention.
- Anxiety.
- Depression.
What Are the Stages of Lewy Body Dementia (LBD)?
Lewy body dementia, sometimes misspelled as Louie body dementia, is a progressive disease. On average, people with LBD live five to eight years from diagnosis to death.
In the early stages, people with LBD can still live an everyday life.
As the disease advances, their movement and thinking abilities deteriorate, and they need more and more help from others.
In the later stages, people with LBD may depend on others for their living activities, like feeding and bathing.
How About a Lewy Body Dementia Diagnosis?
There is no one test that a doctor can use to reach a definite diagnosis.
A diagnosis is typically made based on a person’s medical history, family history, and the presentation of symptoms.
A physical exam, neuropsychological testing, and brain imaging tests may also be used to help rule out other causes of dementia.
Lewy Body Dementia Treatment
The primary focus of Lewy body disease treatment is to manage symptoms, which may include medication and therapy.
Medication
There is no specific medication that has been proven to be effective in treating Lewy body dementia.
However, certain medications may be prescribed to help manage symptoms, such as:
- Cholinesterase inhibitors for delusions.
- Antidepressants for depression.
- Carbidopa-levodopa is used to treat movement problems associated with Lewy body Parkinson’s disease.
Therapy
Non-medication approaches include:
Modifying the environment to help people with dementia function more effectively, for example, by removing clutter and noise.
Creating a daily routine and breaking tasks into simple steps that are easy to follow.
Tips for Family and Caregivers
- Be patient.
- Be flexible with activities and expectations as the person’s abilities change over time.
- Allow for more rest periods, even during the day.
- Encourage socialization and physical activity to help reduce anxiety and depression.
- Try not to argue or correct a person who is hallucinating; instead, redirect their attention.
- Develop routines that can help anchor the person in reality, such as regularly scheduled meals, baths, and relaxation times.
- Stick to simple explanations, such as using simpler words and keeping questions concise.
- Reduce distractions in your environment, for example, bright lights.
- Organize information from doctors and other care providers so the person can review it later on their own.
- Discuss any changes in the person’s behavior with your doctor.
- Join support groups for caregivers to share experiences and emotional support.
Chapter 5. Vascular Dementia
Strokes typically cause vascular dementia.
The symptoms depend on what parts of the brain are damaged.
Like other types of dementia, it takes patience and empathy to take good care of our loved ones.
Let’s learn together.
By Bessi from Pixabay
What Are the Causes of Vascular Dementia?
Vascular dementia results from damage to the brain’s blood vessels that supply oxygen and nutrients. This can occur due to stroke, mini-strokes, or other conditions that reduce blood flow to the brain.
Changes in the brain include small areas of dead tissue (multi-infarct dementia), bleeding, and changes in the structure of blood vessels.
These changes can lead to problems with thinking, memory, and other cognitive functions.
Risk factors are the same as those for stroke, including high blood pressure, diabetes, smoking, and high cholesterol.

Image by Yunus GÜREL from Pixabay
Smoking is not suitable for your health…
What Are the Symptoms of Vascular Dementia
Depending on which functioning area of the brain is affected, people with vascular dementia may have different symptoms.
However, common symptoms include problems with thinking and memory, as well as difficulties with planning and carrying out tasks—for example, trouble paying bills, getting lost, and misplacing items.
Other symptoms may include changes in mood and behavior, such as depression, agitation, and anger.

Image by Wolfgang Eckert from Pixabay
I don’t know what I am doing
What Are the Stages of Vascular Dementia
The stages of vascular dementia can vary depending on the underlying cause, but typically involve a gradual decline in cognitive function.
Early-stage symptoms may include difficulty with planning and executive function, as well as problems with short-term memory.
As the condition progresses, patients may experience difficulties with language, visuospatial skills (such as drawing, buttoning shirts, and making a bed), and motor function.
In the late stages of vascular dementia, patients may be unable to care for themselves and require 24-hour supervision.
What About the Diagnosis of Vascular Dementia
There is no definitive test to diagnose vascular dementia.
A diagnosis of vascular dementia may be made based on a review of the person’s medical history, a physical examination, and laboratory tests.
A brain scan (CT or MRI) may also be done to look for evidence of stroke or other abnormalities in the brain.
Treatment of Vascular Dementia
The goal of treatment is to improve the quality of life and maintain independence as long as possible. Treatment may include:
Medications to treat underlying conditions, such as hypertension or diabetes.
Cholesterol-lowering drugs help prevent further damage to the blood vessels.
Antiplatelet medications, such as aspirin, help prevent blood clots from forming.
Antidepressants or antipsychotic medications treat mood and behavior changes.
Occupational, physical, and speech therapy help with daily activities and communication.
Other things that are worth trying are:
Physical activity: Exercise is beneficial for people with vascular dementia. It can help improve blood flow to the brain and reduce the risk of further damage to blood vessels.
Cognitive rehabilitation: This therapy can help people with vascular dementia learn new ways to compensate for their cognitive impairments. It can also help them learn how to better manage their condition.
Tips for Family and Caregivers
The care for someone with vascular dementia will vary depending on the individual’s specific situation and needs.
However, some general tips include:
Learning as much as possible about the condition. This can help you better understand what your loved one is going through and how you can give the best support.
Encouraging your loved one to stay active and engaged in activities they enjoy. This can help reduce boredom and frustration, and may slow the progression of the condition.
Helping them stick to a healthy diet and exercise routine. It improves blood flow to the brain and potentially slows the progression of vascular dementia.
Providing emotional support and understanding. Dealing with a cognitive decline can be very difficult and distressing, and your empathy can brighten your loved one’s day.
Seeking supportive care. It can include counseling, respite care, and other services to help make life easier for the person with vascular dementia and their caregivers.
Chapter 6. Other Forms of Dementia
Other than those four significant types of dementia mentioned above, there are other ones:
Childhood dementia,
Alzheimer’s among the Down Syndrome population,
And, of course, alcoholic dementia.
So, drink at your own risk…
Childhood Dementia
Contrary to common beliefs, dementia can happen to any age group. Childhood dementia (or Childhood Alzheimer’s) is progressive brain damage occurring in young people, from infants to teenagers.

Sanfilippo syndrome. Wikipedia.
Children get this type of dementia from birth. Some of the 70 rare genetic disorders that lead to childhood dementia are:
- Inborn errors of metabolism
- Lysosomal disorders
- Mucopolysaccharidoses
- Peroxisomal disease
- Leukodystrophy
Every year in the world, 1 in 2800 newborns has one of these genetic disorders.
Just like the adult form of dementia, kids with childhood dementia have similar symptoms:
- Memory loss
- Confusion
- Difficulty learning new information
- Difficulty remembering information that was learned in the past
- Difficulty communicating
- Difficulty with motor skills
- Behavior changes
- Personality changes
- Sleep problems
In addition, they may have other symptoms of specific genetic disorders that cause childhood dementia, such as:
- Seizures
- Vision and hearing problems
- Problems with their bones and joints
- Issues with their heart, lungs, and intestines
Some children may experience an early onset of symptoms as infants, while others start to exhibit symptoms in their teenage years.
The progression of childhood dementia varies from a few months to decades. As more and more brain areas are damaged, these kids gradually lose all their bodily functions.
In the end, most children die before turning 18.
Mixed Dementia
Mixed dementia is a condition where a person has brain changes from more than one form of dementia.
Alzheimer’s disease occurring with vascular dementia accounts for more cases than other causes. The physical changes include abnormal protein deposits and blood vessel problems in the brain that co-occur.
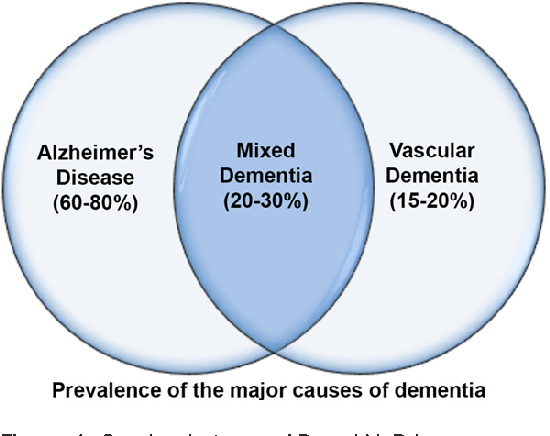
Symptoms of mixed dementia may vary depending on which part of the brain is damaged.
There is no cure for mixed dementia, but drugs may be prescribed to treat the symptoms.
Autoimmune Dementia
Confusion, seizures, memory loss, and behavioral changes are typical symptoms of autoimmune dementia.
The condition is caused by the immune system attacking the brain. Autoimmune dementia is often wrongly diagnosed as a neurodegenerative or psychiatric condition.

Image by Ulrike Mai from Pixabay
Errr…it is more than just biting your own tail…
Autoimmune diseases that cause this type of dementia are:
- Multiple sclerosis
- Systemic lupus erythematosus
- Behçet’s disease
- Sjögren’s syndrome
People with autoimmune dementia often start at a relatively young age.
Treatment for autoimmune dementia generally involves corticosteroid treatment or plasma exchange.
Autoimmune dementia may be a form of reversible dementia.
Korsakoff Dementia
Wernicke-Korsakoff syndrome (WKS) is a neurodegenerative disorder caused by a severe thiamine (vitamin B1) deficiency, mainly from eating disorders, malnutrition, and alcohol abuse.
It has a nickname: “Wet Brain.”

Can I call you “Wet Brain”?
Vitamin B1 deficiency can cause brain damage, leading to increased difficulty with memory, movement, vision, and coordination.
It could be a form of reversible dementia.
WKS consists of two distinct stages: Wernicke’s encephalopathy and Korsakoff syndrome.
Wernicke’s encephalopathy (Wernicke’s brain disease) results from damage to specific brain areas, such as the thalamus and hypothalamus. It occurs suddenly and could be life-threatening.
The symptoms include increased confusion and problems in vision, balance, and movement.
Korsakoff syndrome, on the other hand, usually develops slowly after Wernicke’s encephalopathy. It is caused by damage to small areas in the middle region of the brain.
WKS can be prevented by abstaining from alcohol or, at least, by drinking alcohol in moderation.
A balanced diet that includes foods rich in vitamin B1 can also help prevent the development of WKS—for example, whole grains, nuts, seeds, beans, lean meats, and certain vegetables.
Huntington’s Dementia
Huntington’s dementia is a rare type of dementia due to a defective gene on chromosome 4.

Huntington’s disease. Wikipedia.
Left:
Normal brain.
Right:
Hungtington’s
The telltale sign of Huntington’s disease is uncontrolled movement of the arms, legs, head, face, and upper body.
Symptoms also include a decline in thinking and reasoning skills:
- Memory
- Concentration
- Judgment
- Ability to plan and organize
Most people with Huntington’s disease eventually need help with daily activities ( bathing, dressing, eating, etc.).
Many people with Huntington’s disease live in specialized long-term care facilities or nursing homes.
The outlook for people with Huntington’s disease is currently poor. Most people with Huntington’s die within 15 to 20 years of diagnosis.
However, new treatments and an improved understanding of the disease offer hope for the future.
Primary Progressive Aphasia
Primary progressive aphasia (PPA dementia) is a rare neurological syndrome affecting a person’s communication ability. It is a type of frontotemporal dementia.
Primary progressive aphasia is characterized by the loss of the ability to speak, write, and understand written or spoken language.
It is caused by shrinking certain brain sections responsible for speech and language.

Primary progressive aphasia. Wikipedia.
Language regions

Affected language region
CT scan
People with primary progressive aphasia may initially have problems with communication but eventually will lose the ability to care for themselves and need day-to-day care.
Parkinson’s Disease Dementia
Parkinson’s disease dementia (PDD) is a type of dementia that occurs in some people with Parkinson’s disease.
PDD can cause problems with thinking, memory, and behavior.
People with PDD may have trouble remembering, making decisions, or controlling emotions.
They may also have changes in their sleep patterns and mood.

Credit: National Library of Medicine
The symptoms of PDD usually start after the age of 60. The disorder is more common in men than women.
It is not clear what causes PDD, but it is thought to be related to changes in the brain that occur with Parkinson’s disease.
There is no cure for PDD, but medications, therapy, and support groups can help manage the symptoms.
Down Syndrome and Alzheimer’s Disease
People with Down syndrome have an extra copy of chromosome 21. They have a significantly higher risk of developing a type of dementia very similar to Alzheimer’s disease.

Credit: National Institutes on Aging
Symptoms of Alzheimer’s in people with Down syndrome may include:
- Reduced interest in being sociable.
- Decreased enthusiasm for usual activities.
- A decline in the ability to pay attention.
- Changes in personality and behavior.
It is challenging to tell if a person with Down syndrome has dementia.
Just think about it: how do you assess a person’s thinking-skill changes when they have intellectual disabilities?
Some people with Down syndrome will eventually develop dementia, and there is no way to prevent that.
Creutzfeldt-Jakob Disease(CJD)
Creutzfeldt-Jakob disease is a rare and fatal brain disorder, and the chance of getting it is about one in a million worldwide.
CJD usually affects people over 60 and occurs in both men and women.
The cause of CJD is believed to be related to abnormally folding prion proteins that destroy brain cells.
Symptoms of CJD include dementia, memory loss, impaired vision, impaired coordination, and muscle twitching.
As the disease progresses rapidly, patients may experience seizures, coma, and death within 8 months on average.
It was sometimes mistakenly called CJD dementia.
There is no cure for CJD, and treatment is focused on relieving symptoms and providing supportive care.
Alcoholic Dementia
Alcoholic dementia, or alcohol-related dementia (ARD), is a type of dementia caused by excessive drinking over the years.
Alcohol directly affects brain cells, resulting in problems with memory, learning, and other cognitive skills.

Credit to Fotorech and ulleo from pixabay
Drinking can really make you stupid. :p
The Wernicke-Korsakoff syndrome is a syndrome of alcohol-related dementia.
Surprisingly, a person with this type of dementia may have little ability to learn new things. However, many of their other mental skills are still highly functioning.
Alert
They are capable of creating believable stories to cover up their memory gaps.
At the late stage, they may develop a problem with motor skills, and the most common causes of death are cancer and bacterial infections.
While alcohol-related dementia can happen in young people, it’s often seen in older adults.
Early treatment is the key.
Patients can significantly improve their condition for the early stage of alcoholic dementia by quitting alcohol and eating a balanced diet.
Chapter 7. Progression of Dementia & Alzheimer’s Disease
People with dementia usually go through mild, moderate, and severe stages.
However, the exception is early-onset Alzheimer’s disease.
And rapidly progressive dementia.
Let’s examine care strategies at all stages of the disease.
Various types of dementia progress at different rates, and their symptoms may vary.
But in general, the progression of dementia and Alzheimer’s disease can be divided into three stages: mild, moderate, and severe.
Mild Stage
In the mild stage of dementia, people may experience some early signs of dementia, such as memory loss and difficulty with complex tasks.
They may also struggle to find the right words to express themselves.
People in the mild stage of dementia typically function independently.
Moderate Stage
In the moderate stage of dementia, individuals experience increased difficulty with everyday activities, such as bathing, dressing, and eating.
They may also experience confusion and disorientation.
People in the moderate stage of dementia typically need some help from family or caregivers.
Severe Stage
In the end stage of dementia, people become entirely dependent on others for their care.
They may lose the ability to communicate and risk developing serious health problems such as pneumonia.
Infections are a common cause of death in the final stage of dementia.
The average living time for all types of dementia is about 8 years from diagnosis.
Early Onset Dementia or Alzheimer’s Disease
Alzheimer’s disease is a degenerative brain disease that typically affects older adults. However, in some cases, people may develop the disease at a younger age. This is known as young-onset Alzheimer’s.

Credit to CIHI
People with young-onset Alzheimer’s often face unique challenges.
For example, others may question their diagnosis.
Most would think dementia is an old person’s disease. Can a young person also have it? Seriously?
They may also have problems in relationships or at work because they are not performing as expected.
They suddenly become the worst boyfriend, girlfriend, or coworker.
So it’s essential to get an accurate diagnosis.
Their family and caregivers will gain a better understanding of the situation, and they will have more time to make financial and legal arrangements.
Rapidly Progressive Dementia
Dementia is a progressive condition that gets worse over time.
The rate of deterioration varies among individuals, but the decline can be sudden and rapid for some.
This is called rapidly progressive dementia (RPD).
RPD is rare but progresses quickly, often over weeks or months, and can quickly become fatal.

Many conditions may cause RPD, including Alzheimer’s, strokes, Parkinson’s, infections, prion disease, and cancer.
Quick diagnosis and proper treatment may reverse some cases of RPD.
For example, cancer, hormone imbalance or metabolic disturbances, and infections are often treatable, and in these cases, RPD is reversible.
Unfortunately, most cases of RPD have no cure. The treatment goal is to reduce distress, maintain comfort, and improve quality of life.
Providing Care During the Progression
Here are some helpful tips for individuals with dementia and their families to cope better while providing care throughout the progression of the disease.
Self-Administered Gerocognitive Exam (SAGE)
SAGE is a cognitive test that laypeople can administer, designed to detect early signs of dementia.
The SAGE test has four parts:
- A memory test assesses immediate and delayed recall of words.
- A language test assesses a person’s ability to name objects, follow commands, and repeat words and phrases.
- A visuospatial test assesses the ability to draw objects and copy geometric shapes.
- An executive function test assesses the ability to plan, organize, and complete tasks.
The SAGE test takes approximately 10-15 minutes to complete.
The highest score is 22. A score lower than 17 is considered abnormal. You will need to see a specialist for further evaluation.
Maintaining Joy Through Stages of Dementia
Finding ways to maintain joy throughout the stages of dementia is essential.
Simple things such as spending time with loved ones, listening to music, or being outdoors can be enjoyable moments in this stressful time.
Many activities can also help people with dementia stay engaged and connected to others. For example, helping with laundry or preparing meals.
Self-Regulation Tools To Combat Boredom and Loneliness
Many self-regulation tools can help people with dementia combat boredom and loneliness.
Even dementia care at home can utilize these tools:
Music therapy: Listening to music or playing an instrument can help people with dementia relax and feel joy.
Art therapy, including drawing, painting, or sculpting, can help people with dementia express themselves and connect with others.
Reminiscence therapy: Discussing past experiences can help individuals with dementia feel connected to their life stories.
Pet therapy: Interacting with animals can help individuals with dementia reduce stress and feel more calm.
Palliative Care for Dementia
A palliative approach to care is a person-centered approach that aims to provide comfort and improve the quality of life for people with an incurable illness.

Image by ???? Use at your Ease ???????? from Pixabay
It is not dependent on the time left to live and can be started early in a patient’s illness trajectory.
Palliative care can be used for people with any stage of dementia, including pain relief, improving quality of life, and supporting family and caregivers.
Talk to your doctor, case manager, and healthcare professionals for more information.
End-of-Life Care
EOL care is at the final phase of life when the patient has only hours, days, or weeks to live.
The patient’s care plan is adjusted based on their needs at EOL, which may include pain and symptom control.

Image by ???? Use at your Ease ???????? from Pixabay
As the patient’s condition advances, they may require increased or total assistance with personal care and mouth care and may sleep most of the day and night.
Family and caregivers can provide support by ensuring that the person is comfortable and has access to pain relief.
Professional home care, memory care, and nursing homes can relieve burdens on the family.
Talk to your doctor, case manager, and healthcare professionals for more information.
Chapter 8. Dementia Treatment
There are no cures for dementia.
But there are ways to minimize the adverse effects and provide maximum comfort.
Let us dive in.
Image by InspiredImages from Pixabay
The best treatment for dementia will vary depending on the individual’s specific situation and needs.
The goal is not to cure Alzheimer’s or dementia but to manage symptoms and provide support throughout the disease.

Image by PublicDomainPictures from Pixabay
Some general tips for treating dementia may include:
1. Creating a supportive and safe environment: This may involve ensuring the person with dementia has a safe place to live, with easy access to medical care and support from family and friends.
2. Promoting social and recreational activities: Staying active and engaged can help slow the progression of dementia and improve quality of life.
3. Managing medical conditions: Treating underlying medical conditions like hypertension or diabetes can help manage dementia symptoms.
4. Medications: There are several medications available that can help improve cognitive function and slow the progression of dementia.
- Cholinesterase inhibitors: These medications can help improve cognitive function by increasing levels of acetylcholine. It is a chemical essential for memory and learning.
- Memantine: This medication can help improve cognitive function and delay the progression of dementia.
- Antipsychotic medications can help reduce aggression, agitation, and delusions.
- Antidepressant medications: These medications can help improve mood and sleep.
5. Nutritional support: Eating a healthy diet and getting adequate nutrition can help improve brain function and overall health.
6. Respite care: Taking breaks from caregiving can help reduce stress and burnout.
7. Memory care: a type of long-term care for people with Alzheimer’s, dementia, and other cognitive impairments.
Memory care facilities help residents maintain their cognitive and physical abilities by offering:
- Higher level of care than assisted living facilities.
- With 24-hour supervision and security.
- Specialized activities and therapies.
Chapter 9. Dementia Prevention
Can you prevent dementia?
The short answer is “No”.
However, there are steps you can take to maintain your brain health…
Image by Arek Socha from Pixabay
You cannot prevent Alzheimer’s disease, but you can do things that may help reduce the risk, such as:
- Staying mentally and physically active throughout your life.
- Staying socially engaged and having a robust social network.
- Eating healthy, exercising regularly, and controlling your blood pressure and cholesterol.
- Taking supplements, such as vitamin E, omega-3 fatty acids, and ginkgo Biloba, may also help reduce your risk of Alzheimer’s.
Research also indicates that consistent short sleep duration reduces the risk of dementia. So, getting 7 to 9 hours of sleep daily improves your brain health.
Clinical trials are ongoing to test new treatments and preventive measures for Alzheimer’s. Participating in a clinical trial is one way to contribute to advancing Alzheimer’s research.
Conclusion
Congratulations! You have reached the end of this post. Let’s do a little recap.
We started by explaining dementia and Alzheimer’s disease, then proceeded to show the characteristics of four major types of dementia (Alzheimer’s disease, frontotemporal lobe dementia, Lewy body dementia, and vascular dementia).
We also visited other rare types of dementia.
The information in this post is by no means exhaustive.
It takes months of learning and practice, and then you can confidently say you are providing good care for your loved ones.
I hope this post marks the beginning of that journey.
Or a simple reference.
Is there any additional information I should include, or are there any errors in this post? Please comment below!