[lwptoc]
Introduction: Navigating the Diabetes Labyrinth
Are you ready to dive deep into the enigmatic world of diabetes, a condition that impacts millions around the globe? Well, you’re in the right place!
We’ve curated the ultimate, all-encompassing guide to unravel the mysteries of diabetes. We’ll uncover everything from its various types and origins to mastering the art of managing and thriving with it.
So, strap in and prepare to be enlightened as we embark on this eye-opening odyssey together!

Types of Diabetes – One Name, Many Faces
Diabetes comes in various shapes and sizes, like a chameleon changing colors. Let’s unmask the different types of diabetes:

Blue Circle of Diabetes
Type 1 Diabetes: The Unwelcome Attack on Beta Cells
Type 1 diabetes is an autoimmune condition, which means the body’s immune system turns against its own cells, specifically the insulin-producing beta cells in the pancreas. With these cells under siege, the pancreas struggles to produce enough insulin, leading to elevated blood sugar levels.
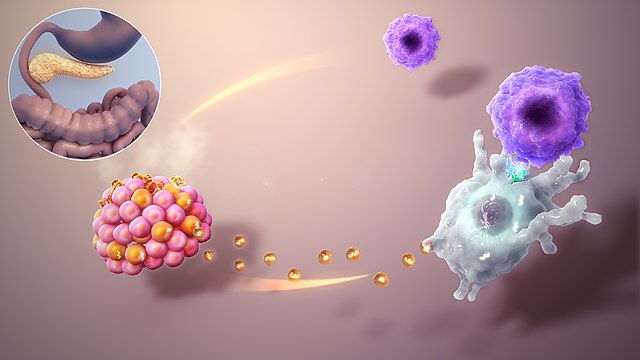
Autoimmune attack in type 1 diabetes. In wikipedia
Type 1 diabetes accounts for approximately 5-10% of all diabetes cases. It typically develops during childhood or adolescence, though it can appear at any age.
The exact cause of this autoimmune response remains a mystery. Still, researchers believe a combination of genetic and environmental factors, such as viral infections, might be at play.
Unfortunately, type 1 diabetes is a lifelong condition requiring daily management through insulin injections or an insulin pump, along with regular blood sugar monitoring, a balanced diet, and exercise.
Type 2 Diabetes: The Insidious Insulin Resistance
Type 2 diabetes, the most common form of diabetes, affects 90-95% of people with the condition.
In this case, the body either doesn’t produce enough insulin or becomes resistant to its effects, resulting in elevated blood sugar levels. The onset of type 2 diabetes is usually gradual and often goes undetected for years.
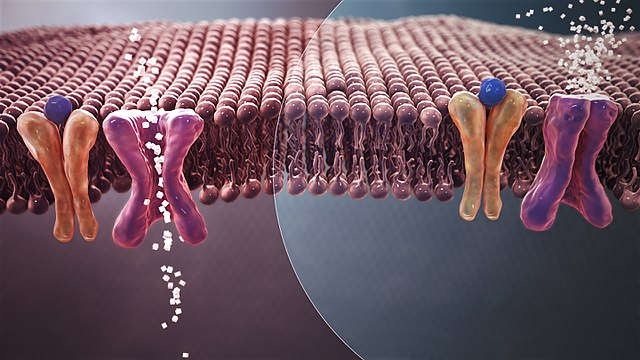
“Reduced insulin secretion or weaker effect of insulin on its receptor leads to high glucose content in the blood.” In wikipedia
Risk factors for type 2 diabetes include obesity, physical inactivity, genetics, and older age.
Unlike type 1 diabetes, type 2 can sometimes be managed through lifestyle changes, such as adopting a healthy diet, increasing physical activity, and losing weight.
However, some individuals may require oral medications or insulin therapy to control optimal blood sugar.
Gestational Diabetes: The Pregnancy Predicament
Gestational diabetes is a temporary form of diabetes that occurs during pregnancy, affecting approximately 2-10% of expectant mothers.
Pregnant women naturally experience some insulin resistance, but those with gestational diabetes struggle to produce enough insulin to counteract this resistance, resulting in high blood sugar levels.
While gestational diabetes typically resolves after giving birth, it increases the risk of developing type 2 diabetes for both the mother and child later in life.
Managing gestational diabetes involves:
- Monitoring blood sugar levels.
- Adopting a healthy diet.
- Exercising regularly.
- Sometimes using insulin therapy.
MODY: The Uncommon Inheritance
Maturity Onset Diabetes of the Young (MODY) is a rare, genetically inherited form of diabetes, accounting for just 1-2% of all cases. It usually manifests before the age of 25.

It is caused by a mutation in a single gene, disrupting insulin production or function. There are several subtypes of MODY, each resulting from a different genetic mutation.
MODY is often misdiagnosed as type 1 or type 2 diabetes due to its rarity and overlapping symptoms.
Treatment varies depending on the subtype but may include oral medications, insulin injections, or lifestyle changes.
LADA: The Late Bloomer
Latent Autoimmune Diabetes in Adults (LADA) is an autoimmune form of diabetes that develops later in life, usually after age 30.
LADA shares features of both type 1 and type 2 diabetes, sometimes referred to as “type 1.5” diabetes.
The autoimmune destruction of beta cells is slower in LADA than in type 1 diabetes. Individuals with LADA may initially be misdiagnosed as having type 2 diabetes.
Risk factors for LADA are similar to those for type 1 diabetes, including genetics and environmental triggers.
Treatment for LADA typically involves lifestyle changes and oral medications initially. Still, as beta cell destruction progresses, insulin therapy becomes necessary.
🫑
In short, understanding the differences between these types of diabetes can help inform appropriate diagnosis, treatment, and management strategies, ultimately improving the quality of life for those affected by the condition.
Causes and Risk Factors – The Diabetes Recipe
What are the ingredients that make up the diabetes recipe? Let’s explore the causes and risk factors:
Genetics: A Dicey Inheritance
Genetics plays a crucial role in determining an individual’s risk of developing diabetes.
A family history of diabetes, particularly in the case of type 1, MODY (Maturity Onset Diabetes of the Young), and LADA (Latent Autoimmune Diabetes in Adults), can significantly increase your chances of being affected by the condition.
Genetic mutations or predispositions can be passed down through generations, affecting how your body produces or responds to insulin.
Lifestyle Factors: The Unhealthy Trio
Poor diet, physical inactivity, and smoking can contribute significantly to developing type 2 diabetes.
Consuming excessive amounts of unhealthy foods, such as processed items high in sugar and unhealthy fats, can lead to weight gain and insulin resistance.
On the other hand, regular physical activity helps maintain a healthy weight and improve insulin sensitivity.
Smoking exacerbates insulin resistance and increases the risk of cardiovascular complications associated with diabetes.
Obesity: The Weighty Culprit
Obesity, particularly excess weight around the abdomen, is a significant risk factor for type 2 diabetes.
Excess fat, especially visceral fat (the fat surrounding your internal organs), can cause inflammation and hormonal imbalances that lead to insulin resistance.

Losing weight and maintaining a healthy body mass index (BMI between 18.5 and 24.9) can significantly reduce the risk of developing type 2 diabetes and improve blood sugar control for those already diagnosed with the condition.
Insulin Resistance: The Stubborn Roadblock
Insulin resistance is a condition where the body doesn’t use insulin effectively, often leading to type 2 diabetes.
When cells become resistant to insulin’s effects, the pancreas compensates by producing more insulin. Over time, the pancreas may struggle to keep up, resulting in elevated blood sugar levels.
Factors contributing to insulin resistance include obesity, poor diet, physical inactivity, and certain medications. Addressing these factors can help prevent or manage type 2 diabetes.
Autoimmune Destruction of Beta Cells: The Unseen Battle
Autoimmune destruction of beta cells, the insulin-producing cells in the pancreas, is a critical factor in type 1 diabetes and LADA.
In both cases, the immune system mistakenly attacks these cells, impairing insulin production and leading to elevated blood sugar levels.
The exact cause of this autoimmune response is still unclear. Still, researchers believe a combination of genetic and environmental factors, such as viral infections, might trigger this process.
Unfortunately, once beta cells are destroyed, insulin production cannot be restored, necessitating lifelong insulin therapy.
Ethnicity: The Disproportionate Impact
Certain ethnic groups, such as African Americans, Hispanics, and Native Americans, have a higher risk of developing diabetes.
This increased risk can be attributed to genetic, lifestyle, and socioeconomic factors.
For example, these populations may have a higher prevalence of obesity, which contributes to insulin resistance and type 2 diabetes. Additionally, disparities in healthcare access and quality can further exacerbate the problem.
Public health initiatives tailored to these communities can help reduce the incidence and impact of diabetes among these populations.
🍠
All in all, understanding the various risk factors for diabetes is vital in order to identify those at risk, implement appropriate prevention strategies, and ensure optimal management for those already living with the condition.
A combination of genetic and lifestyle factors can contribute to diabetes risk, and addressing these issues through targeted interventions can make a significant difference in the lives of those affected.
Symptoms and Diagnosis – Reading the Diabetes Tea Leaves
How do you know if diabetes is knocking at your door?

Look out for these symptoms:
Frequent urination, excessive thirst, increased hunger, fatigue, blurred vision, and slow-healing wounds are common symptoms of diabetes, signaling elevated blood sugar levels. When insulin production or function is impaired, glucose accumulates in the bloodstream, resulting in these symptoms.
Frequent urination (polyuria) occurs when the kidneys work overtime to remove excess glucose from the blood, increasing urine production. This, in turn, can cause excessive thirst (polydipsia) as the body tries to replenish lost fluids.
Increased hunger (polyphagia) is a response to the body’s inability to use glucose effectively, depriving cells of energy and triggering hunger signals.
Fatigue in diabetes results from a combination of factors, including high blood sugar levels, dehydration, and the body’s inability to utilize glucose efficiently.
Blurred vision arises from high blood sugar levels, causing the eye’s lens to swell, altering its shape and focusing ability.
Lastly, slow-healing wounds can occur due to poor circulation, nerve damage, and impaired immune function, all of which are consequences of uncontrolled diabetes.
Confirming the Diagnosis: Key Tests
To confirm a diabetes diagnosis, healthcare providers rely on several tests to accurately gauge blood sugar levels:
A1C Test: The A1C test, also known as the HbA1c or glycated hemoglobin test, measures your average blood sugar levels over the past 2-3 months. It provides a more stable, long-term view of blood sugar control than daily glucose checks. An A1C level of 6.5% or higher on two separate tests indicates diabetes.
Fasting Plasma Glucose Test: The fasting plasma glucose test checks your blood sugar after an overnight fast, typically requiring 8-12 hours without food or drink (except water). A fasting blood sugar level of 126 mg/dL (7.0 mmol/L) or higher on two separate tests suggests diabetes.
Oral Glucose Tolerance Test: The oral glucose tolerance test gauges blood sugar levels before and after drinking a sugary liquid. Blood sugar is tested initially after an overnight fast and then again at 2-hour intervals after consuming the glucose solution. A 2-hour blood sugar level of 200 mg/dL (11.1 mmol/L) or higher indicates diabetes.
Sometimes, healthcare providers may use a random plasma glucose test, which measures blood sugar levels without regard to when the individual last ate. A random blood sugar level of 200 mg/dL (11.1 mmol/L) or higher, along with symptoms, can indicate diabetes.
By and large, recognizing the symptoms of diabetes and seeking prompt diagnosis through appropriate testing is crucial for effective diabetes management. Early detection and intervention can help prevent or delay the onset of diabetes-related complications, improving the quality of life for those affected.
Diabetes Complications: The Ripple Effect
Diabetes can have far-reaching consequences on various aspects of health, leading to a range of complications if left uncontrolled. Some of the most common complications include:
Diabetic Retinopathy
High blood sugar levels can damage the delicate blood vessels in the retina, the light-sensitive tissue at the back of the eye responsible for vision.
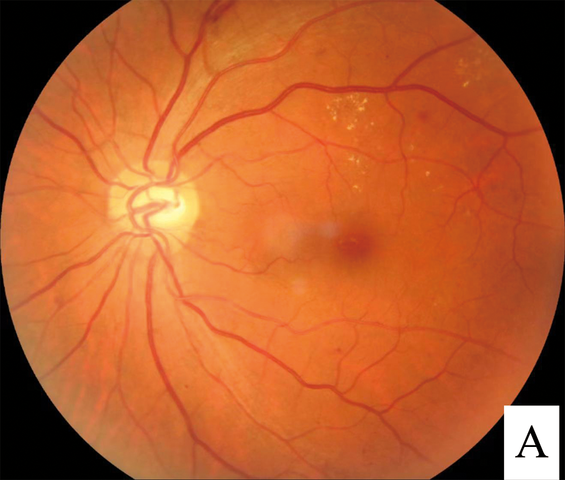
By Shaofeng Hao, Changyan Liu, Na Li, Yanrong Wu, Dongdong Li, Qingyue Gao, Ziyou Yuan, Guanyan Li, Huilin Li, Jianzhou Yang, and Shengfu Fan. – (2022). “Clinical evaluation of AI-assisted screening for diabetic retinopathy in rural areas of midwest China“. PLoS One 17 (10): e0275983. DOI:10.1371/journal.pone.0275983. PMID 36227905. PMC: 9560484. Figure 1, panel A, CC BY 4.0, Link
This damage can cause the vessels to leak, swell, or even close off, potentially leading to vision loss. In advanced stages, the growth of abnormal blood vessels can cause further damage, even blindness.
Early detection and management of blood sugar levels can help prevent or slow the progression of diabetic retinopathy.
Diabetic Neuropathy
Prolonged high blood sugar levels can cause nerve damage, often resulting in pain, numbness, or weakness in the extremities, particularly the feet, and legs.
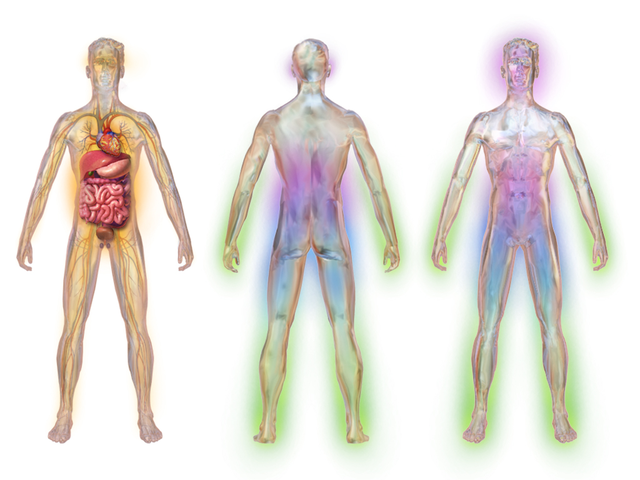
“Illustration depicting areas affected by diabetic neuropathy” From wikipedia
This condition, known as diabetic neuropathy, can also affect the digestive system, urinary tract, blood vessels, and heart.
Managing blood sugar levels and a healthy lifestyle can help prevent or slow the progression of neuropathy.
Diabetic Nephropathy
Diabetes can damage the kidneys, impairing their ability to effectively filter waste from the blood.
Over time, this can lead to diabetic nephropathy, progressing to kidney failure if left untreated.
Early detection and management of blood sugar levels, blood pressure, and kidney function can help prevent or slow the progression of diabetic nephropathy.
Cardiovascular Disease
Diabetes increases the risk of heart attack, stroke, and other heart-related complications due to its impact on blood vessels and the likelihood of other risk factors such as high blood pressure, high cholesterol, and obesity.
Maintaining good blood sugar control, adopting a heart-healthy lifestyle, and working closely with healthcare providers can help minimize the risk of cardiovascular disease in people with diabetes.
Peripheral Arterial Disease
Diabetes can contribute to the narrowing or blockage of blood vessels in the legs, a condition called peripheral arterial disease (PAD).
It can lead to poor circulation, increasing the risk of infections, ulcers, and delayed wound healing. In severe cases, PAD can necessitate amputation.
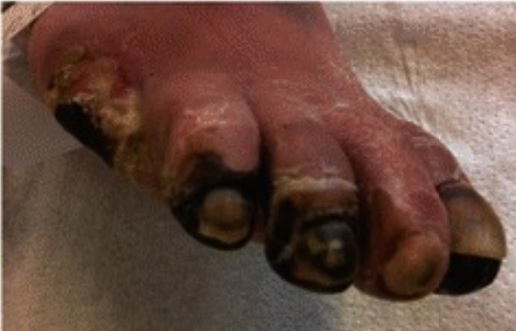
“Peripheral arterial disease resulting in necrosis of multiple toes” From wikipedia
Smoking cessation, regular exercise, and proper foot care are essential for reducing the risk of PAD and its complications.
Foot Complications
Diabetic neuropathy and poor circulation can cause foot problems, such as ulcers, infections, and deformities.
In extreme cases, these issues may lead to amputation.
Regular foot exams, proper foot care, and prompt treatment of any problems can help prevent severe foot complications.
🥜
The bottom line is while diabetes can lead to a range of complications, many of these issues can be prevented or managed through diligent blood sugar control, a healthy lifestyle, and regular medical checkups.
Early detection and intervention are critical in minimizing the impact of these complications on overall health and quality of life.
Diabetes Management: Tools and Strategies for Optimal Control
Managing diabetes involves a combination of tools and strategies to keep blood sugar levels within the target range. Critical components of diabetes management include:
Blood Glucose Monitoring
Regularly checking your blood sugar levels is essential for staying on track and making necessary adjustments.
Monitoring can help you understand how different factors, such as food, exercise, and stress, affect your blood sugar levels. It also informs treatment decisions, such as adjusting insulin doses or oral medications.
Insulin Therapy
For people with type 1 diabetes, and sometimes those with type 2 diabetes, insulin therapy is crucial for regulating blood sugar levels. 💉💉💉
Insulin can be administered through injections or an insulin pump. The type, dose, and timing of insulin may vary depending on individual needs and lifestyle factors.
Oral Medications
For managing type 2 diabetes, oral medications may help control blood sugar levels.
These pills work in various ways, such as increasing insulin production, improving insulin sensitivity, or reducing glucose production in the liver. The choice of medication depends on the individual’s specific needs and overall health.
Diet and Nutrition
Eating a balanced diet is crucial for maintaining stable blood sugar levels.
A diet rich in whole grains, fruits, vegetables, lean proteins, and healthy fats can help prevent blood sugar spikes and support overall health.
Consulting with a registered dietitian or certified diabetes educator can help tailor dietary choices to individual needs and preferences.
Exercise and Physical Activity
Regular physical activity can improve insulin sensitivity and help control blood sugar levels.
Exercise can also contribute to weight loss, lower blood pressure, and reduce the risk of heart disease.
It’s essential to consult with healthcare providers to develop a safe and effective exercise plan tailored to individual needs and abilities.
Weight Management
Maintaining a healthy weight is crucial for reducing the risk of diabetes complications and improving overall health.
Weight management strategies may include dietary changes, increased physical activity, and behavioral modifications, such as setting realistic goals and seeking support from friends or professionals.
Continuous Glucose Monitoring (CGM)
A CGM device measures blood sugar levels throughout the day, providing real-time data to inform decision-making.
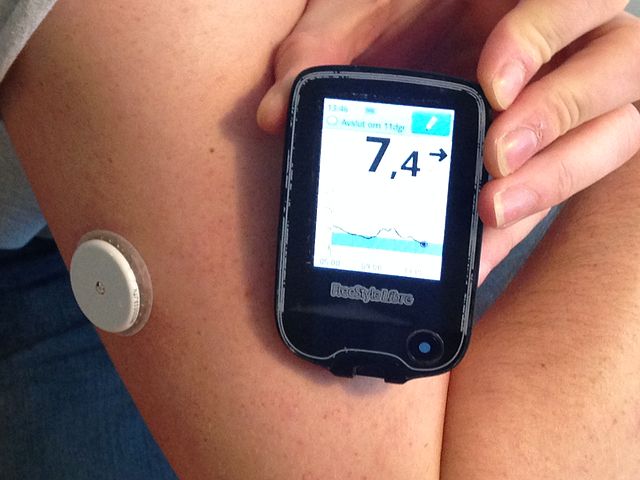
Abbott Laboratories’ FreeStyle CGM From wikipedia
The device consists of a sensor inserted under the skin and a transmitter that sends data to a display device.
CGM can help identify patterns, detect trends, and provide alerts for high or low blood sugar levels.
Insulin Pumps
Insulin pumps are small devices that deliver a continuous supply of insulin, helping to maintain optimal blood sugar control.
The pump is typically worn on the body and connected to a small tube that delivers insulin through a tiny needle inserted under the skin.
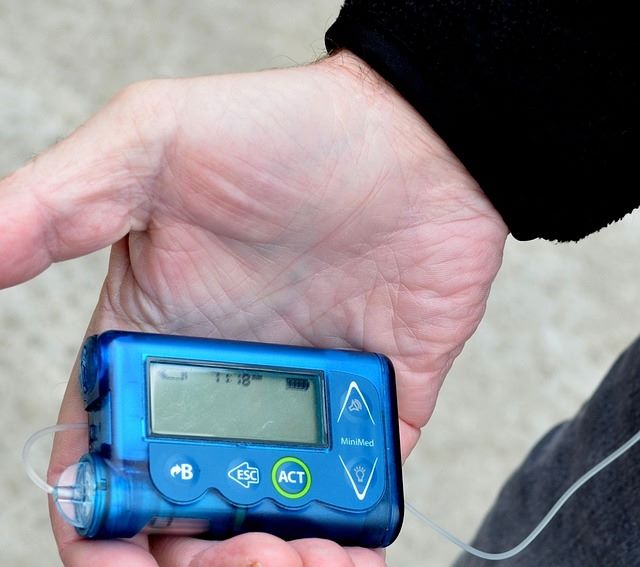
Image by jwskks5786 from Pixabay
Insulin pumps can be programmed to provide different insulin doses at specific times, offering more precise control and flexibility than injections.
🫑
Finally, effective diabetes management involves a combination of tools and strategies tailored to individual needs.
By monitoring blood sugar levels, adjusting treatment plans, and maintaining a healthy lifestyle, people with diabetes can reduce the risk of complications and enjoy a better quality of life.
Diabetes Prevention and Lifestyle Changes – Your Diabetes Shield
Diabetes is a growing global health concern, but the good news is that you can take steps to prevent or delay its onset. Adopting specific lifestyle changes can build a shield against diabetes and improve your overall health. Here are six essential strategies to consider:
Identifying and Addressing Prediabetes
Prediabetes is a condition where blood sugar levels are higher than normal but not yet high enough to be classified as type 2 diabetes.
Catching prediabetes early and taking action can help prevent or delay the onset of type 2 diabetes. Lifestyle changes, such as improving your diet, increasing physical activity, and losing weight, can significantly impact reversing prediabetes.
Maintaining a Healthy Weight
Achieving and maintaining a healthy weight is crucial for reducing the risk of developing diabetes.
Excess weight, particularly around the abdomen, can contribute to insulin resistance and increase the likelihood of type 2 diabetes.
By adopting a balanced diet and engaging in regular physical activity, you can work towards a healthy weight and lower your risk.
Regular Physical Activity
Exercise plays a vital role in diabetes prevention.
Regular physical activity can improve insulin sensitivity, help maintain a healthy weight, and contribute to overall health.
Aim for at least 150 minutes of moderate-intensity aerobic exercise or 75 minutes of vigorous-intensity aerobic exercise per week, combined with strength training exercises two or more days per week.
Balanced Diet
A nutrient-rich, balanced diet is essential for maintaining stable blood sugar levels and reducing the risk of diabetes.
Focus on consuming whole grains, fruits, vegetables, lean proteins, and healthy fats while limiting processed foods, added sugars, and unhealthy fats.
Consulting with a registered dietitian or certified diabetes educator can help you create a personalized meal plan that meets your nutritional needs and preferences.
Smoking Cessation
Quitting smoking can significantly lower the risk of diabetes and improve overall health.
Smoking contributes to insulin resistance and raises blood sugar levels, increasing the likelihood of developing type 2 diabetes.
Seek support from healthcare providers, friends, or smoking cessation programs to help you kick the habit for good.
Stress Reduction
Chronic stress can negatively impact blood sugar levels, potentially increasing the risk of diabetes.
Managing stress through relaxation techniques, mindfulness, and other coping strategies can help prevent blood sugar spikes and promote overall well-being.
Consider practicing deep breathing, meditation, yoga, or engaging in hobbies that bring you joy to help manage stress.
******
To wrap things up, adopting these lifestyle changes can help you build a shield against diabetes and improve your overall health.

By focusing on early identification, maintaining a healthy weight, engaging in regular physical activity, adopting a balanced diet, quitting smoking, and managing stress, you can significantly reduce your risk of developing diabetes and enjoy a better quality of life.
The Future of Diabetes: Groundbreaking Advancements and Research
The management of diabetes has come a long way over the years. With continuous research and technological advancements, the future looks even more promising.
Here are five groundbreaking developments that could revolutionize diabetes care in the coming years:
Artificial Pancreas: A Game-Changer for Blood Sugar Control
The artificial pancreas, a closed-loop system, significantly advances diabetes management.
This device combines an insulin delivery pump with continuous glucose monitoring (CGM) to automate blood sugar control. By continuously adjusting insulin delivery based on real-time glucose levels, the artificial pancreas can maintain blood sugar levels within a target range, minimizing the risk of hypoglycemia and hyperglycemia.
Several artificial pancreas systems have already received regulatory approval, and ongoing research aims to refine further and improve their performance.
This technology could significantly reduce the burden of diabetes management and improve the overall quality of life for people with diabetes.
Stem Cell Research: Unlocking the Potential for Regenerating Beta Cells
Stem cell research holds immense potential for diabetes treatment, particularly for type 1 diabetes.
Scientists are investigating the possibility of using stem cells to regenerate insulin-producing beta cells destroyed by the immune system in people with type 1 diabetes.
By restoring the body’s ability to produce insulin, stem cell therapy could potentially cure or significantly improve diabetes management.
While still in the experimental phase, early studies have shown promising results. The ongoing research aims to develop safe and effective stem cell therapies that could revolutionize diabetes treatment.
Islet Cell Transplantation: Restoring Insulin Production
Islet cell transplantation is a procedure that involves transplanting healthy islet cells from a donor pancreas into a person with type 1 diabetes.
These transplanted cells can potentially restore the body’s ability to produce insulin, reducing or eliminating the need for insulin injections.
Although still a relatively rare and complex procedure, islet cell transplantation has shown promising results in some patients.
Ongoing research focuses on improving the success rate, reducing the risk of complications, and developing alternative sources of islet cells, such as stem cells or bioengineered tissues.
New Medications: Expanding the Arsenal for Blood Sugar Control
Developing new medications is crucial in improving diabetes management and reducing the risk of complications.
Researchers are continually working on novel drugs that target different aspects of blood sugar control, such as improving insulin sensitivity, increasing insulin secretion, or slowing down carbohydrate absorption.
These new medications can offer additional options for blood sugar control, particularly for people who do not respond well to existing treatments or experience side effects.
The ongoing research aims to bring safer and more effective drugs to the market, further enhancing diabetes management.
Diabetes Apps and Wearables: Revolutionizing Self-Management
Diabetes apps and wearable devices have transformed the way people manage their conditions.
These tools offer unparalleled convenience and insights, from tracking blood sugar levels and physical activity to providing reminders for medications and appointments.
Some diabetes apps can even analyze your data and provide personalized recommendations to help you achieve better blood sugar control.
Wearable devices, such as CGMs and smartwatches, offer real-time data and alerts, enabling people with diabetes to make informed decisions about their care.
As technology advances, we can expect even more sophisticated and user-friendly diabetes apps and wearables to emerge, further revolutionizing self-management and empowering people with diabetes to take control of their health.
🍒🍒🍒🍒🍒🍒
To summarize, the future of diabetes care looks promising, with groundbreaking advancements and research paving the way for improved management and potentially even a cure.
From artificial pancreas systems and stem cell research to islet cell transplantation, new medications, and innovative digital tools, the landscape of diabetes treatment is evolving rapidly.

The Psychological Side of Diabetes: Navigating the Emotional Landscape
Living with diabetes isn’t just about managing blood sugar levels and making lifestyle adjustments; it’s also about navigating the complex emotional landscape of a chronic condition.
From diabetes distress and mental health challenges to coping mechanisms and support groups, let’s explore the psychological aspects of living with diabetes.
Diabetes Distress: The Emotional Burden of a Chronic Condition
Diabetes distress refers to the emotional burden that comes with managing diabetes, which can manifest as feelings of frustration, anger, guilt, or even hopelessness.
The constant need to monitor blood sugar levels, make dietary choices and remember medications can be overwhelming and lead to emotional exhaustion.
It’s essential to recognize that diabetes distress is a natural response to the challenges of living with a chronic condition. Acknowledging and addressing these emotions through healthy coping strategies can help alleviate the distress and improve overall well-being.
Depression and Anxiety: Mental Health Challenges for People with Diabetes
People with diabetes are more likely to experience depression and anxiety. Studies indicate they are two to three times more likely to suffer from these conditions than the general population.
The reasons behind this increased risk are multifaceted, including the emotional burden of managing diabetes, the impact of blood sugar fluctuations on mood, and the social stigma that sometimes comes with chronic illness.
Depression and anxiety can negatively impact diabetes self-management, making it more challenging to maintain blood sugar control and adhere to treatment plans. Addressing these mental health challenges is crucial by seeking professional help and adopting healthy coping mechanisms.
Coping Mechanisms: Strategies for Managing Emotional Distress
Developing healthy coping strategies can help individuals with diabetes better manage emotional distress and improve their overall quality of life. Some effective coping mechanisms include:
Practicing mindfulness: Mindfulness techniques, such as meditation or deep breathing exercises, can help reduce stress and improve emotional well-being.

Seeking therapy: Talking to a mental health professional, such as a psychologist or therapist, can provide guidance and support in managing emotional challenges related to diabetes.
Setting realistic goals: Breaking down diabetes management tasks into smaller, achievable goals can reduce feelings of overwhelm and help build a sense of accomplishment.
Engaging in self-care: Prioritizing self-care activities, such as getting enough sleep, exercising, and engaging in hobbies, can help improve mood and overall well-being.
Support Groups: The Power of Connection
Support groups provide a safe space for people with diabetes to connect with others who share similar experiences, offering invaluable emotional support and practical advice.
By sharing stories, challenges, and successes, individuals can gain new perspectives and learn from the experiences of others.
You can find support groups in person and online, catering to different preferences and needs. Some groups are condition-specific, focusing on type 1 or type 2 diabetes.
In contrast, others may cater to specific demographics, such as parents of children with diabetes or adults with a recent diagnosis.
🍆
Ultimately, living with diabetes involves more than just physical health; it also encompasses the emotional and psychological aspects of managing a chronic condition. By acknowledging the emotional challenges, adopting healthy coping strategies, and seeking support from others, individuals with diabetes can improve their mental well-being and overall quality of life.
Living with Diabetes – Thriving, Not Just Surviving
Living with diabetes can be challenging, but with the proper knowledge, resources, and mindset, you can thrive and maintain a high quality of life.
From diabetes education and self-management to navigating travel, work, and health insurance, let’s explore strategies for making life with diabetes more manageable and fulfilling.

Diabetes Education: Knowledge is Power
Education is crucial for optimal diabetes self-care. Understanding the different aspects of diabetes management, treatment options, and potential complications empowers you to make informed decisions about your care.
Resources such as healthcare providers, diabetes educators, books, and online sources can provide a wealth of information and guidance.
Self-Management: Taking Charge of Your Diabetes Care
Taking an active role in your diabetes care is essential for maintaining good health. Effective self-management involves:
- Regular blood sugar monitoring to track your levels and make adjustments as needed.
- Medication management, including taking prescribed medications and insulin as directed.
- Implementing lifestyle adjustments, such as maintaining a balanced diet, exercising regularly, and practicing stress-reduction techniques.
- Regularly attending medical appointments and discussing any concerns with your healthcare team.
Traveling with Diabetes: Plan for a Stress-Free Trip
Traveling with diabetes requires some extra planning and preparation. Before embarking on a trip, consider the following:
- Pack a sufficient supply of medications, insulin, and blood sugar testing supplies, as well as any necessary snacks and emergency supplies, such as glucose tablets or a glucagon kit.
- Keep your medical supplies in your carry-on luggage to avoid lost or damaged items.
- Inform your travel companions about your diabetes and what to do in case of an emergency.
- Research the availability of healthcare services at your destination and carry a list of local healthcare providers
Workplace Accommodations: Managing Diabetes on the Job
Managing diabetes at work can be challenging, but discussing your needs with your employer and requesting reasonable accommodations can help you stay healthy and productive.
Possible accommodations may include:
- Flexible scheduling to allow for regular blood sugar monitoring, medication administration, and snack breaks.
- A private area for insulin injections or blood sugar testing if needed.
- Permission to attend medical appointments during work hours.
Remember, under the Americans with Disabilities Act (ADA), employers must provide reasonable accommodations for employees with disabilities, including diabetes.
Health Insurance Considerations: Navigating Coverage and Resources
Understanding your health insurance coverage and exploring available resources can help you make informed decisions about your diabetes care. Consider the following:
- Review your health insurance policy to understand what diabetes-related services and supplies are covered.
- Compare the costs of different treatment options and medications, as well as any available generic alternatives.
- Look for financial assistance programs, such as co-pay assistance cards or patient assistance programs, to help with the cost of medications and supplies.
Utilize resources like diabetes educators, support groups, and online forums to gather information and share experiences with others with diabetes.
🍅
In a nutshell, thriving while living with diabetes involves physical health and equipping yourself with knowledge and resources to navigate various aspects of life.
By seeking diabetes education, practicing self-management, planning for travel, advocating for workplace accommodations, and understanding health insurance considerations, you can take control of your diabetes and live a fulfilling life.
Diabetes in Special Populations – Unique Challenges, Tailored Solutions
Diabetes affects millions worldwide, but some populations face unique challenges and require tailored approaches to manage their condition effectively.
Let’s look closely at diabetes in children, the elderly, pregnant women, and athletes and explore the strategies necessary to support their specific needs.
Diabetes in Children: Building a Foundation for a Healthy Life
Children with diabetes, particularly those with type 1 diabetes, face unique challenges compared to adults. These challenges can impact their physical, emotional, and social well-being.
Some of the critical difficulties children with diabetes face include the following:
Developmental considerations: Children’s bodies and insulin needs change as they grow. Adjusting insulin dosages and managing blood sugar levels can be more complicated in children due to growth spurts, puberty, and hormonal fluctuations.
Treatment adherence: Children may need help to follow a strict treatment regimen, including frequent blood sugar testing, insulin injections, or the use of an insulin pump, and maintaining a consistent meal plan.
They may also need help with carbohydrate counting and understanding the impact of physical activity on blood sugar levels.
Emotional and psychological challenges: Children with diabetes may feel isolated or different from their peers, leading to embarrassment, anger, or depression.
They may also experience anxiety about their condition and fear of complications, such as hypoglycemia or long-term health problems.
School-related issues: Diabetes management can be challenging in a school setting, requiring coordination between the child, parents, teachers, and school staff. Ensuring the child has access to a safe environment for blood sugar testing, insulin administration, and proper nutrition can be challenging.
Family dynamics: Diabetes can stress the entire family, as parents and siblings may need to adapt to new routines, dietary restrictions, and concerns about the child’s health.
Parents may feel overwhelmed or guilty, and siblings may experience feelings of jealousy or resentment.
Peer pressure and social situations: Children with diabetes may feel left out in social situations, especially if their friends don’t understand the importance of their diabetes management.
They may also face peer pressure to engage in unhealthy behaviors, such as skipping insulin injections or consuming sugary treats.
Limited independence: Unlike their peers, children with diabetes may have little autonomy due to the constant need for blood sugar monitoring and insulin administration. It can lead to feelings of frustration and a desire for more independence.
Long-term complications: Children with diabetes have an increased risk of developing complications later in life, such as heart disease, kidney disease, neuropathy, and retinopathy. Early and consistent management of the condition is crucial to minimize these risks.
Support from healthcare professionals, parents, teachers, and peers is crucial in helping children with diabetes navigate these challenges and lead healthy, fulfilling lives.

Critical considerations for managing diabetes in children include:
- Collaborating with healthcare providers to develop a personalized care plan that addresses the child’s growth, development, and activity levels.
- Encouraging open communication with the child about their feelings and experiences related to diabetes.
- Teaching the child age-appropriate self-management skills, such as blood sugar monitoring, insulin administration, and making healthy food choices.
- Providing emotional support and encouragement to help the child cope with the demands of living with diabetes.
Diabetes in the Elderly: Balancing Treatment and Quality of Life
Elderly individuals with diabetes face unique challenges due to age-related factors and comorbidities.
The key challenges they face include the following:
Age-related physiological changes: The elderly experience changes in kidney function, body composition, insulin sensitivity, and hormonal balance. These factors can make diabetes management more complex, with a higher risk of hypoglycemia and hyperglycemia.
Comorbidities: Older adults with diabetes are more likely to have other chronic health conditions, such as heart disease, hypertension, kidney disease, or cognitive decline. These comorbidities can complicate diabetes management and increase the risk of complications.
Polypharmacy: Elderly individuals with multiple health conditions often take several medications, which can interact with diabetes medications and increase the risk of side effects or complications.
Cognitive decline and dementia: Cognitive impairment can make it difficult for older adults to manage their diabetes, including adhering to medication schedules, monitoring blood glucose levels, and making appropriate lifestyle choices.
Mobility and physical limitations: Older adults may have reduced mobility and physical function, making engaging in regular physical activity more challenging, an essential aspect of diabetes management.
Vision and dexterity problems: Older adults may experience difficulties with vision, making it hard to read glucose meters or insulin pumps. Dexterity issues can make administering insulin injections more challenging.
Nutritional challenges: Older adults may have difficulty maintaining a balanced diet due to changes in appetite, dental issues, or problems in meal preparation. Malnutrition or inadequate nutrient intake can negatively impact blood glucose control.
Social isolation and emotional well-being: Elderly individuals with diabetes may experience loneliness, depression, or anxiety related to their condition, affecting their overall well-being and ability to manage diabetes effectively.
Financial constraints: Limited income or financial resources can make it challenging for older adults to afford medications, glucose monitoring supplies, and healthy food choices.
Age-specific treatment goals: Diabetes management goals should be individualized for elderly patients, considering their overall health status, life expectancy, and risk of complications. Overly aggressive treatment may increase the risk of hypoglycemia and other adverse outcomes.
Healthcare providers, caregivers, and family members should work together to support elderly individuals with diabetes in managing their condition, considering their unique challenges and needs.
A tailored approach to care and frequent monitoring can help optimize diabetes management and minimize the risk of complications.

Critical aspects of diabetes care for old adults include:
- Adjusting treatment goals to balance blood sugar control with the risk of hypoglycemia and other complications.
- Considering the impact of comorbidities and medications on diabetes management.
- Regularly assessing cognitive function, as cognitive decline can impact the ability to perform self-management tasks.
- Collaborating with caregivers and healthcare providers to ensure appropriate support and resources are available.
Diabetes during Pregnancy: Ensuring a Healthy Mother and Baby
Pregnant women with diabetes, including both pre-existing diabetes (type 1 or type 2) and gestational diabetes, face unique challenges due to the effects of pregnancy on glucose metabolism and the potential impact of diabetes on maternal and fetal health.
The key challenges they face include the following:
Blood glucose control: Maintaining tight blood glucose control is crucial during pregnancy to reduce the risk of complications for both the mother and baby. Pregnant women with diabetes must frequently monitor their blood sugar levels and adjust their medications and insulin dosages accordingly.
Insulin resistance: Hormonal changes during pregnancy can increase insulin resistance, particularly in the second and third trimesters. It may require adjustments to insulin dosages and increased monitoring to maintain optimal glucose control.
Medication adjustments: Some diabetes medications may not be safe during pregnancy. Women with pre-existing diabetes may need to switch to insulin or adjust their oral medications under the guidance of their healthcare providers.
Risk of hypoglycemia: Tight glucose control can increase the risk of hypoglycemia (low blood sugar), which can be dangerous for both the mother and baby. Pregnant women with diabetes must be vigilant about monitoring their blood sugar levels and promptly treating hypoglycemia.
Dietary management: Pregnant women with diabetes must follow a balanced diet that provides essential nutrients for the baby’s growth and development while maintaining optimal blood glucose control. They may need to work closely with a registered dietitian or nutritionist to develop an individualized meal plan.
Increased risk of complications: Diabetes during pregnancy increases the risk of maternal complications, such as preeclampsia and preterm labor, as well as fetal complications, including macrosomia (large birth weight), congenital anomalies, and neonatal hypoglycemia. Careful monitoring and management are essential to minimize these risks.
Prenatal care and monitoring: Pregnant women with diabetes require frequent prenatal care appointments and additional monitoring, such as fetal ultrasounds and non-stress tests, to ensure the baby’s well-being.
Postpartum challenges: After delivery, women with pre-existing diabetes need to adjust their insulin dosages and medications, while those with gestational diabetes should be monitored for the development of type 2 diabetes. Additionally, breastfeeding may require further adjustments to insulin dosages and glucose monitoring.
Emotional stress: Managing diabetes during pregnancy can be stressful, as the responsibility of maintaining tight blood glucose control and the potential impact on the baby’s health can cause anxiety, fear, and guilt.
Pregnant women with diabetes should work closely with their healthcare providers, including obstetricians, endocrinologists, and dietitians. This collaboration helps develop a comprehensive care plan to manage diabetes effectively during pregnancy and minimize the risk of complications.

Managing diabetes during pregnancy involves:
- Collaborating with a healthcare team, including obstetricians, endocrinologists, and diabetes educators, to develop a tailored care plan.
- Monitoring blood sugar levels closely and adjusting insulin dosages as needed to maintain optimal control.
- Following a balanced diet to meet the nutritional needs of both the mother and the developing baby.
- Regularly attending prenatal appointments and monitoring the baby’s growth and development.
Diabetes in Athletes: Striving for Peak Performance
Athletes with diabetes, whether they have type 1 or type 2 diabetes, face unique challenges due to the effects of physical activity on glucose metabolism and the need for careful management to optimize performance and maintain good health.
The key challenges they face include the following:
Blood glucose control: Physical activity can cause fluctuations in blood glucose levels, making it difficult for athletes with diabetes to maintain optimal control. Exercise can cause blood glucose to either rise or fall, depending on factors such as the type, duration, and intensity of the activity, as well as the individual’s insulin sensitivity and carbohydrate intake.
Hypoglycemia risk: Intense or prolonged exercise can increase the risk of hypoglycemia (low blood sugar) in athletes with diabetes, especially those using insulin.
To prevent hypoglycemia, athletes may need to adjust their insulin dosages, consume additional carbohydrates, or monitor their blood glucose levels more frequently during and after exercise.
Hyperglycemia risk: High-intensity or competitive sports can cause a surge in stress hormones, temporarily increasing blood glucose levels. Athletes with diabetes may need to adjust their insulin dosages or other medications to prevent hyperglycemia (high blood sugar).
Insulin adjustments: Athletes with diabetes who use insulin need to carefully adjust their dosages based on their exercise routine, intensity, and duration. It may involve reducing basal insulin rates, adjusting bolus insulin for meals, or using different types of insulin to accommodate their training schedule.
Nutrition management: Athletes with diabetes must carefully plan their meals and snacks to provide adequate energy and nutrients while maintaining good blood glucose control. It may involve carbohydrate counting, monitoring the glycemic index of foods, and adjusting meal timing around exercise sessions.
Dehydration risk: Diabetes can increase the risk of dehydration, impairing athletic performance and increasing the risk of heat-related illnesses. Athletes with diabetes should be vigilant about maintaining adequate hydration before, during, and after exercise.
Monitoring and technology: Athletes with diabetes may benefit from continuous glucose monitoring (CGM) systems, which can provide real-time feedback on blood glucose levels during exercise and help guide insulin and nutrition adjustments.
Awareness and communication: Athletes with diabetes need to inform their coaches, teammates, and trainers about their condition and educate them on the signs and symptoms of hypoglycemia and hyperglycemia, as well as the appropriate actions to take in case of an emergency.
Recovery and rest: Athletes with diabetes should pay attention to their recovery and rest, as inadequate recovery can negatively impact blood glucose control and increase the risk of injury.
By working closely with their healthcare providers and sports nutritionists, athletes with diabetes can develop individualized strategies for managing their blood glucose levels, insulin dosages, and nutrition plans to optimize their athletic performance and maintain good health.

Critical strategies for managing diabetes in athletes include:
- Developing a personalized exercise plan that takes into account the athlete’s specific sport, training schedule, and blood sugar control needs.
- Regularly monitoring blood sugar levels before, during, and after exercise to prevent hypoglycemia and hyperglycemia.
- Adjusting insulin dosages and carbohydrate intake to account for increased energy expenditure during physical activity.
- Collaborating with healthcare providers, coaches, and trainers to ensure a comprehensive support system is in place.
🥕
To wind things up, addressing the unique challenges faced by children, the elderly, pregnant women, and athletes with diabetes is crucial for ensuring their overall health and well-being.
By recognizing and addressing the specific needs of these populations, healthcare providers, caregivers, and individuals with diabetes can work together to develop tailored strategies that promote optimal diabetes management and quality of life.
Conclusion: The Journey Continues
As we reach the end of our comprehensive diabetes journey, we hope this guide has provided you with valuable insights and resources.
Remember, knowledge is power, and understanding the many facets of diabetes can help you navigate the labyrinth confidently.
Keep exploring, stay informed, and embrace the journey toward better health and well-being!









