[lwptoc]
1. Introduction
Imagine a life in your golden years, where radiant smiles and hearty laughter are the norms, meals are enjoyed without discomfort, and conversations flow with crystal clear articulation.
The key to this vibrant picture? Stellar oral health.
Often relegated to the periphery of our wellness concerns, oral health plays an indispensable role in shaping the quality of life for seniors, transcending the superficial confines of aesthetics and discomfort.
It fuels efficient nutrition by enabling adequate mastication, fosters interpersonal communication through articulate speech, and may even be instrumental in mitigating the risk of various chronic ailments.
Yet, like an ominous cloud on a sunny day, aging ushers in a slew of potential dental issues. These creeping threats, left unaddressed, can escalate into grave concerns, casting a pall over oral well-being and systemic health.
This post ventures into the often-navigated terrains of dental dilemmas typical in older adults. It seeks to illuminate the reasons behind their onset and arm you with robust, pragmatic strategies for proactive management.
After all, your golden years should radiate with the blush of health, unmarred by the gloom of dental distress!

Image by Yves Yoseph from Pixabay
2. The Prevalence of Dental Problems in Older Adults
As we age, we become more susceptible to various health challenges, and dental health is no exception.
According to the Centers for Disease Control and Prevention (CDC), nearly 70% of adults aged 65 and older have some form of periodontal disease. This serious gum infection damages gums and can destroy the jawbone.
Furthermore, the World Health Organization (WHO) reports that oral diseases pose a significant health burden for many countries, affecting people throughout their lifetime, causing pain, discomfort, disfigurement, and even death.
Why is the prevalence of dental problems exceptionally high among older adults?
The reasons are multi-fold:
- Aging predisposes individuals to dental issues as teeth wear down over time and become more susceptible to decay and damage.
- Certain medical conditions common in older age, such as diabetes, can affect oral health.
- Medications that older adults often need to take for other health conditions can also impact oral health by causing dry mouth, for instance.
Hence, being aware of this susceptibility and taking proactive steps toward dental health is crucial to managing health in the golden years.
3. Dental Problem #1: Tooth Decay
As we embark on our journey into understanding dental issues prevalent among older adults, tooth decay stands out as one of the most common culprits.
Tooth decay, also known as cavities or caries, is caused by harmful bacteria that feast on the sugars in our food, producing acid. Over time, these acids can erode the tooth’s protective outer layer, the enamel, leading to decay.
We find ourselves more prone to cavities with age, not just because we might have developed a sweet tooth over the years.
One key reason is dry mouth, which many older adults face due to medications for common conditions like high blood pressure or depression.
Saliva plays a critical role in neutralizing the acids produced by bacteria, and its reduction means that these acids can run rampant, leading to tooth decay.
Cavities in older adults may not be as evident as those in younger individuals. They commonly occur around older fillings or on the root surfaces of teeth. These parts might not be as noticeable or easily accessible when brushing. Hence, older adults and their caregivers need to be extra vigilant.
Combatting tooth decay requires a multi-pronged approach.
A well-rounded oral hygiene routine must incorporate twice-daily brushing with fluoride toothpaste, regular flossing, and routine dental check-ups.
For those experiencing dry mouth, sipping water throughout the day, avoiding sugary or acidic foods and drinks, and speaking to your healthcare provider about potentially adjusting your medication can be beneficial.
However, tooth decay is not an inevitable part of aging. By understanding the risks and taking appropriate preventative measures, older adults can maintain their dental health and keep that radiant smile for years.
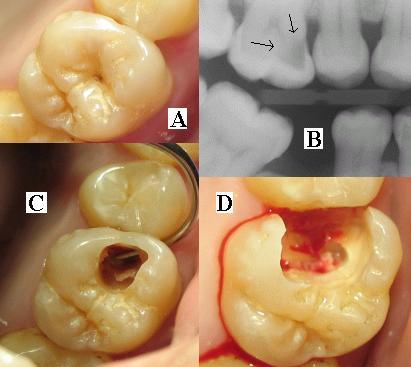
Tooth decay. (2023, May 31). In Wikipedia.
4. Dental Problem #2: Gum Disease
Gum disease is next on our list of dental concerns that predominantly affect older adults
Often overlooked, gum disease, or periodontal disease, is an infection of the tissues that hold your teeth in place. Poor oral hygiene typically allows plaque—a sticky film of bacteria—to build up on the teeth and harden.
In older adults, the prevalence of gum disease escalated, with factors such as years of plaque build-up and decreased immunity playing a significant role.
The early stage of gum disease, known as gingivitis, is characterized by red, swollen gums that bleed easily.
While gingivitis can be reversed with good oral hygiene and regular dental visits, it can advance to periodontitis if left untreated. This more severe form of gum disease can lead to painful chewing, bad breath, and tooth loss.
Furthermore, research has found a connection between gum disease and other health problems such as heart disease, stroke, and diabetes, making it a matter of overall health, not just oral health.
This correlation, known as the mouth-body connection, emphasizes the importance of maintaining good oral health for general well-being, especially in older adults.
Preventing and treating gum disease involves diligent oral hygiene, regular dental visits, and sometimes professional cleanings to remove hardened plaque.
Regular brushing, flossing, and using an antibacterial mouthwash can go a long way in keeping your gums healthy.
Additionally, a balanced diet rich in vitamins C and E can help boost your immune system, making it easier for your body to fight the bacteria that cause gum disease.
In essence, gum disease is more than a mere inconvenience—it’s a significant health risk. But it’s possible to prevent and manage this condition by being aware of the signs and taking action early.
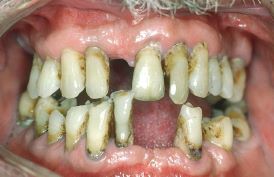
Periodontal disease. (2023, June 13). In Wikipedia.
5. Dental Problem #3: Dry Mouth
Let’s delve into another common dental problem that older adults frequently face: dry mouth or xerostomia.
This condition occurs when the salivary glands do not make enough saliva to keep the mouth wet, leading to a persistently dry feeling in the mouth.
Saliva plays an essential role in oral health, aiding digestion and neutralizing the acids produced by plaque, and washing away dead cells that accumulate on your tongue, gums, and cheeks. If these cells aren’t removed, they can cause mouth sores, infections, and bad breath.
Additionally, saliva helps combat oral microbes, preventing them from multiplying and leading to tooth decay or gum disease.
Therefore, the diminished saliva production that characterizes dry mouth can seriously threaten dental health.
In older adults, dry mouth is often a side effect of medications. With seniors commonly taking multiple medications for various health conditions, the risk of experiencing dry mouth increases.
Other causes include diseases like Sjögren’s syndrome, nerve damage, dehydration, and lifestyle habits like smoking or drinking alcohol.
Some typical signs of dry mouth include a sticky feeling in the mouth, frequent thirst, sores in the mouth, cracked lips, a dry throat, and a burning sensation.
If you notice these symptoms, you must talk to your dentist or doctor, who can help determine the cause and suggest appropriate treatment.
To alleviate dry mouth symptoms, staying hydrated is paramount.
Regular sips of water, sucking on ice chips, or using a mouthwash specially designed for dry mouth can help.
Sugar-free gum or lozenges can stimulate saliva production, and avoiding dehydrating substances like alcohol, caffeine, and tobacco can also be beneficial.
In conclusion, a common but often overlooked issue in older adults is dry mouth. Recognizing its symptoms and implications is the first step in maintaining oral health and quality of life.
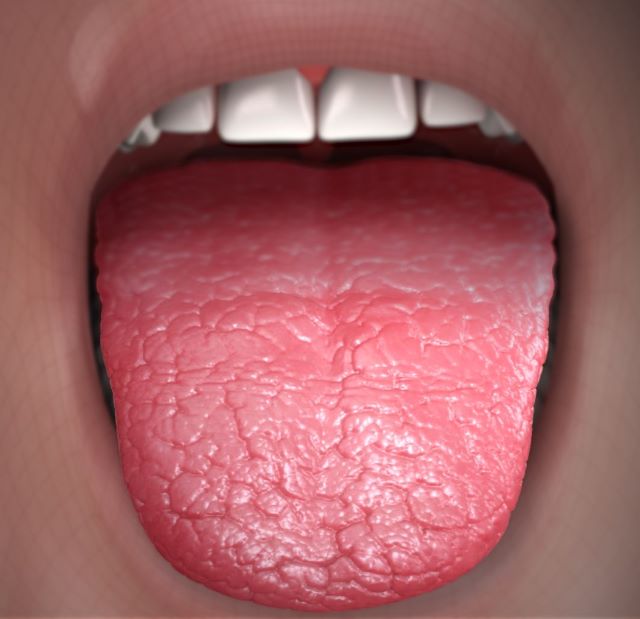
Xerostomia. (2023, April 29). In Wikipedia.
6. Dental Problem #4: Oral Cancer
Digging deeper into our discussion of dental issues that affect older adults, we turn our attention to a more severe problem, oral cancer. While not as common as gum disease or tooth decay, it’s a significant concern due to its potential severity.
According to the American Cancer Society, the average age of most people diagnosed with oral cancer is 62, illustrating its prevalence in older adults.
Oral cancer can occur anywhere in the mouth, including the lips, tongue, cheeks, floor of the mouth, hard and soft palate, sinuses, and pharynx (throat).
It can manifest in various ways, including persistent mouth sores that don’t heal, unexplained bleeding, chronic sore throat or hoarseness, and dramatic weight loss.
One of the main risk factors for oral cancer is tobacco use, including cigarettes, cigars, pipes, and chewing tobacco. Excessive alcohol consumption is another key risk factor. The combination of tobacco and alcohol use significantly increases the risk.
Other risk factors include excessive sun exposure (for lip cancer), a family history of cancer, and being infected with the human papillomavirus (HPV).
Early detection is critical for effective treatment and a better prognosis. Regular dental check-ups are vital since they often include an oral cancer screening. Between visits, individuals should perform self-checks, looking for changes in the oral tissues, unusual lumps, discoloration, or sores that don’t heal.
If oral cancer is detected, treatment options may include surgery to remove the cancerous growth, followed by radiation therapy or chemotherapy to kill any remaining cancer cells. In more advanced cases, targeted drug therapy may be used.
While oral cancer is a severe and potentially life-threatening disease, awareness of its risk factors and symptoms, regular dental check-ups, and early detection can significantly increase survival rates.
It underscores the importance of maintaining good oral hygiene and regular dental visits, especially for older adults.
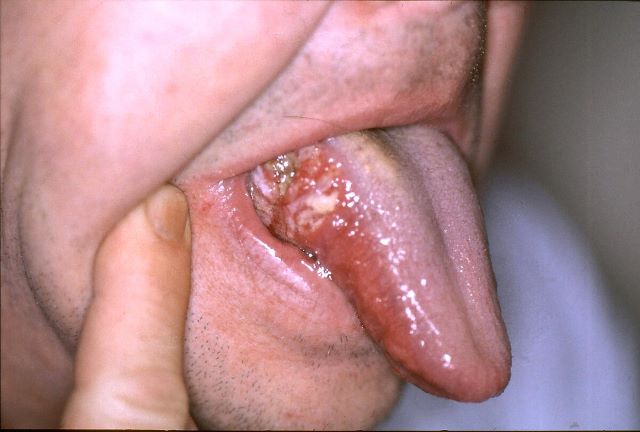
File:ZungenCa2a.jpg. In Wikipedia.
7. Dental Problem #5: Tooth Loss
Another prominent dental issue in older adults is tooth loss, which, though often regarded as a natural part of aging, is more accurately a result of other unchecked dental health problems.
Tooth loss can profoundly impact an individual’s quality of life, affecting not just the aesthetics of their smile but also their ability to speak clearly and consume a healthy, varied diet.
Understanding the causes, implications, and possible solutions is essential for those eager to maintain their dental health in their later years.
Tooth loss can occur due to a variety of reasons.
Poor oral hygiene that leads to gum disease or tooth decay is one of the most common culprits. Chronic illnesses, like diabetes or arthritis, can also make it difficult for individuals to maintain good oral hygiene or compromise the body’s immune response.
The impact of tooth loss extends beyond aesthetics.
It can lead to malnutrition due to difficulty eating various foods. It can also affect an individual’s speech and cause embarrassment or reduced social interactions due to the associated stigma. Moreover, tooth loss can lead to bone loss in the jaw, altering the facial structure and leading to a more aged appearance.
Despite these challenges, there’s hope.
Dental technology has advanced tremendously, offering several solutions for tooth loss. Dentures, bridges, and implants can replace lost teeth, restoring functionality and aesthetics. Dental implants, in particular, provide a long-lasting solution and can help prevent bone loss since they replace the tooth root and the crown.
In conclusion, while tooth loss is a significant concern for older adults, understanding its causes and repercussions, and the solutions available, can empower individuals to take the necessary steps to maintain their dental health and quality of life.
As with all other dental issues, preventive care, regular dental check-ups, and early intervention are critical.
8. The Role of Caregivers in Maintaining Oral Health
Caregivers play a pivotal role in promoting and maintaining the oral health of older adults, especially those with cognitive or physical challenges. Their involvement can help prevent or manage dental problems, contributing significantly to those under their care’s overall well-being and quality of life.
Firstly, caregivers can assist in the daily oral care routine.
This may include brushing and flossing the older adult’s teeth and ensuring they rinse with an antiseptic mouthwash. If applicable, they might also be responsible for cleaning and caring for dentures.
Secondly, caregivers can observe and monitor for any signs of dental problems.
This can range from noticeable discomfort while eating to changes in speech, bad breath, or visible changes in the mouth, teeth, or gums. Early detection of such signs can lead to prompt treatment and prevent complications.
Moreover, caregivers play a crucial role in facilitating regular dental check-ups.
They can schedule appointments, arrange transportation, and provide necessary support during the visit. For individuals with dementia or other cognitive impairments, caregivers can help communicate with the dentist about any changes or concerns.
In essence, caregivers can bridge the gap between older adults and their oral health needs, proactively fighting against common dental issues in this population.

Image by Klaus Hausmann from Pixabay
Conclusion
In conclusion, maintaining good oral health in older adults is integral to overall wellness, directly influencing their quality of life.
Dental problems such as tooth decay, gum disease, dry mouth, oral cancer, and tooth loss are common in this age group but are not inevitable. These issues can be managed or even prevented with consistent and diligent care.
For older adults, especially those with cognitive or physical impairments, caregivers act as the first defense against dental problems.
By assisting with daily oral care routines, monitoring for signs of dental issues, and facilitating regular dental check-ups, caregivers play a pivotal role in supporting the oral health of those in their care.
Remember, oral health matters at every age. By understanding the common dental issues older adults face, we can take steps to address these problems effectively, paving the way for happier, healthier, and more comfortable golden years.


